Back pain in older adults is not always “just ageing.” Sometimes it signals a fracture inside the spine caused by fragile bones. These fractures can lead to severe pain, loss of height, and a stooped posture if untreated.
Understanding the right treatment early can prevent long-term disability. One widely used solution today is kyphoplasty.
Fortunately, Dr Purnajyoti Banerjee offers kyphoplasty in London to patients seeking proper care and guidance for osteoporotic spine fractures.
Today’s blog explains osteoporotic spine fractures, the kyphoplasty procedure and when it is the right choice for patients.
Let’s dive in.
What Are Osteoporotic Spine (Vertebral Compression) Fractures?
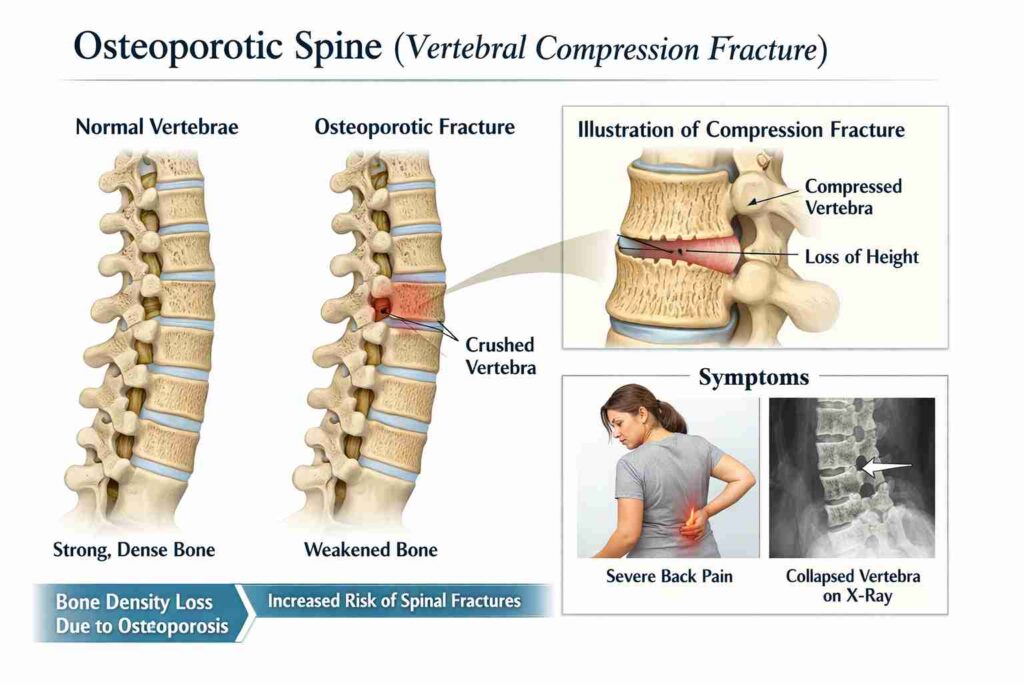
Osteoporotic spine fractures (vertebral compression fractures) occur when weakened vertebrae collapse under normal pressure, sometimes triggered by simple movements such as bending or coughing.
They affect over 1.4 million people worldwide each year and are especially common in adults over 65, particularly women with osteoporosis.[Source] These fractures often cause sudden back pain, height loss, and spinal curvature.
Early diagnosis is important for guiding appropriate treatment for osteoporotic spine fractures, including medications, bracing, and procedures such as kyphoplasty.
How Osteoporosis Leads to Spinal Fractures
Osteoporosis reduces bone density and weakens the internal structure of vertebrae. This makes them unable to handle normal body weight.
Over time:
- Bones become porous and brittle
- Vertebrae gradually lose strength
- Minor stress can cause a sudden collapse
These fractures are sometimes called vertebral compression fractures.
Common Symptoms Patients Experience
The symptoms of spinal compression fractures and osteoporosis can vary widely. Many patients initially mistake them for routine back pain.
Common symptoms include:
- Sudden severe mid or lower back pain
- Pain that worsens when standing or walking
- Height loss over time
- A hunched or forward-bending posture
- Reduced mobility and difficulty bending
Why These Fractures Are Often Misdiagnosed
Many older adults attribute the pain to arthritis or muscle strain. This delays proper vertebral compression fracture treatment. Early imaging often reveals fractures that clinical examination alone cannot detect.
Common reasons for missed diagnosis include:
- Pain develops after minor activity rather than trauma
- Symptoms overlap with routine back pain
- Some fractures cause mild symptoms initially
How Are Osteoporotic Spine Fractures Diagnosed?
Doctors diagnose osteoporotic spinal fractures through a combination of clinical evaluation and imaging tests to confirm the fracture location and determine whether the fracture is recent or old. They first assess symptoms such as back pain patterns, mobility limitations, and any neurological signs.
Dr Purnajyoti Banerjee combines clinical evaluation and imaging to determine an apt treatment plan for osteoporotic spine fractures.
Imaging Tests (X-ray, MRI, CT)
Imaging is essential to confirm a vertebral fracture. Doctors may recommend:
| Imaging Test | Purpose |
| X-ray | Detects collapsed vertebrae |
| MRI | Identifies new fractures and nerve compression |
| CT Scan | Provides detailed bone structure |
Identifying Acute vs Old Fractures
Not every fracture seen on imaging causes pain. Some may be old and already healed.
Doctors analyse:
- Bone marrow changes on MRI
- Fracture shape and vertebral height
- Surrounding tissue inflammation
This step helps determine whether kyphoplasty may help relieve active pain.
Treatment Options for Osteoporotic Spine Fractures
Treatment options range from conservative management to procedures such as kyphoplasty. Many fractures improve with medication, bracing, and physiotherapy.
However, persistent pain may require procedures such as kyphoplasty to stabilise the bone and restore vertebral height.
Conservative (Non-Surgical) Treatment
Doctors usually begin with non-surgical treatment for vertebral fractures. This approach focuses on pain control and natural healing.
Pain meds
Pain medications reduce inflammation and help patients stay active during the healing process.
Common options include:
- Anti-inflammatory medications
- Short-term pain relief medicines
- Bone-strengthening drugs for osteoporosis
Bracing
Bracing is usually temporary and combined with other therapies. Back braces support the spine while fractures heal.
Benefits include:
- Reduced spinal movement
- Improved posture
- Lower pain during daily activities
Physiotherapy
Physiotherapy strengthens muscles supporting the spine. Therapy focuses on:
- Gentle strengthening exercises
- Posture correction
- Balance training
When Conservative Treatment Fails
Unfortunately, not all fractures heal comfortably. Doctors consider further treatment when:
- Pain persists beyond six weeks
- Mobility remains severely limited
- Imaging shows unstable fractures
At this stage, minimally invasive spine surgery for osteoporosis may be recommended.
What Is Kyphoplasty?
The kyphoplasty is a minimally invasive procedure designed to stabilise vertebral fractures using a balloon and bone cement. It restores vertebral height and reduces pain in patients whose fractures do not improve with conservative care.
Step-by-Step Overview of the Procedure
The procedure is performed through a small incision in the back. Imaging guidance ensures accurate placement.
Balloon insertion
A small balloon is inserted into the fractured vertebra. The balloon:
- Creates a small cavity
- Lifts compressed bone
- Restores vertebral height
Cement stabilisation
Once the cavity forms, medical cement is injected. The cement:
- Hardens quickly
- Stabilises the fracture
- Reduces painful movement
Kyphoplasty vs Vertebroplasty
Patients often ask about the kyphoplasty vs vertebroplasty difference.
| Feature | Kyphoplasty | Vertebroplasty |
| Balloon used | Yes | No |
| Height restoration | Possible | Limited |
| Deformity correction | Better | Minimal |
Kyphoplasty often offers better correction of spinal deformity.
When Is Kyphoplasty the Right Choice?
Many ask, ‘when is kyphoplasty recommended?’. Doctors typically recommend kyphoplasty based on pain severity, the age of the fracture, and whether conservative treatments have failed. The best results occur when the fracture is recent and causing severe mobility-limiting pain.
Key Indications for Kyphoplasty
These situations commonly indicate the need for treatment.
Severe persistent pain
Pain that limits walking, sleeping, or daily activities may require intervention.
Failure of 4–6 weeks of conservative care
If pain does not improve with medication, bracing, and physiotherapy, further treatment is considered.
Recent fracture (best outcomes within ~8 weeks)
Earlier treatment often provides better vertebral height restoration. This is why timely evaluation for kyphoplasty is important.
Who Is NOT a Good Candidate?
Kyphoplasty is not recommended for every spinal fracture.
- Mild symptoms: Patients with manageable pain often recover with conservative care.
- Healed fractures: Old fractures that have already stabilised do not benefit from cement stabilisation.
- Infection/instability: Active infection or unstable spinal conditions require different treatment approaches.
Decision-Making Checklist
Doctors evaluate several factors before recommending kyphoplasty.
Key considerations include:
| Factor | Why It Matters |
| Pain severity | Severe pain suggests an unstable fracture |
| Mobility limitation | Difficulty walking or standing |
| Fracture age | Recent fractures respond best |
| Imaging confirmation | MRI confirms active fracture |
This checklist helps determine whether a kyphoplasty procedure is needed.
Benefits of Kyphoplasty
Kyphoplasty can significantly reduce pain, restore vertebral height, and improve mobility. It is considered a safe, minimally invasive spine surgery for osteoporosis when conservative treatment fails.
Pain Relief and Mobility Improvement
Many patients report rapid pain relief within days.
Benefits include:
- Reduced back pain
- Improved walking ability
- Better daily functioning
Restoration of Vertebral Height
Collapsed vertebrae can cause a forward stooped posture.
Kyphoplasty may:
- Restore partial vertebral height
- Improve spinal alignment
- Reduce progressive deformity
Minimally Invasive Advantages
As the incision is small:
- Blood loss is minimal
- Hospital stay is shorter
- Recovery tends to be faster
These advantages make kyphoplasty a valuable option for elderly patients.
Risks and Complications of Kyphoplasty
Although generally safe, no procedure is completely risk-free. Complications are uncommon but can include cement leakage, adjacent fractures, or infection. Careful patient selection significantly reduces these risks.
Cement Leakage
A small amount of cement may leak outside the vertebra. Modern imaging guidance helps minimise this risk.
Adjacent Fractures
Weak bones from osteoporosis may lead to nearby fractures. Bone health management remains essential.
Rare Complications
Experienced surgeons aim to minimise certain risks. Still, these rare risks happen:
- Infection
- Nerve irritation
- Allergic reaction to materials
Recovery After Kyphoplasty
Recovery after kyphoplasty is usually rapid. Many patients return home the same day and resume gentle activity within days. Full recovery depends on bone health and physical rehabilitation.
What to Expect Immediately After
Patients typically:
- Walk within hours of the procedure
- Experience early pain relief
- Return home the same day or the next day
Recovery Timeline
Results vary depending on overall health. Typical recovery milestones:
| Timeline | Recovery Stage |
| 24 hours | Walking comfortably |
| 1 week | Reduced pain |
| 4 weeks | Improved mobility |
Rehabilitation and Lifestyle Changes
Long-term recovery focuses on bone health. Doctors recommend:
- Osteoporosis medications
- Strength and balance exercises
- Fall prevention strategies
Is Kyphoplasty Worth It?

If you are experiencing persistent spinal fracture pain, consult Dr Purnajyoti Banerjee, an experienced spine specialist offering kyphoplasty in London.
Book your consultation today at this email address: purnajyoti74@gmail.com.
People Also Ask
What is the 3-column rule in spine fractures?
The three-column rule classifies spinal stability based on injury to the anterior, middle, and posterior spinal columns. Fractures involving two or more columns are generally considered unstable.
Which procedure treats osteoporotic vertebral fractures?
Minimally invasive procedures such as kyphoplasty or vertebroplasty may be used to stabilise painful osteoporotic vertebral compression fractures when conservative treatments fail.
Is walking good for compression fractures?
Gentle walking may help maintain mobility and circulation during recovery, but activity should follow medical guidance to avoid worsening the fracture.
What happens if L3, L4, or L5 are damaged?
Damage to L3, L4, or L5 vertebrae can cause lower back pain, leg weakness, numbness, or nerve-related symptoms, depending on the severity and the extent of nerve involvement.